What if an invisible energy could both reveal disease and help cure it? From diagnostic scans to targeted cancer therapy, radiation drives some of medicine’s most powerful tools. Understanding how this force can both benefit and harm patients is key to using it safely, responsibly, and to its greatest clinical advantage.

It starts with a click. In a quiet hospital room, a scanner comes to life, revealing what the human eye could never see. That power comes from radiation, a force that helps doctors see, treat, and sometimes even cure disease. From sunlight on the skin to the trace amounts we encounter in hospital scans, radiation is part of our daily lives. It’s unseen, but it matters. The more we understand it, the more safely and wisely we can use it.
Two Kinds of Radiation, Two Very Different Effects
Not all radiation is the same. Think of it like fire: gentle heat can keep you warm, but too much can burn you. Scientists divide radiation into two kinds: non-ionising and ionising.
Non-ionising types, like visible light, radio waves, and microwaves, don’t carry enough energy to damage cells and are generally safe in small doses. On the other hand, ionising radiation, such as X-rays and gamma rays, carries more energy and can harm cells if overused. That might sound worrying, but when handled carefully, this same power helps healthcare professionals diagnose conditions to better lives every single day.
The Dual Nature of Radiation
Medical use of radiation centres on a classic trade-off. For example, a chest X-ray exposes patients to ionising radiation, but it can also reveal a life-threatening condition early, allowing for prompt treatment. That’s why radiology follows the rule of justification: only do the scan if its benefit clearly outweighs any small risk. Interestingly, some research even suggests tiny doses might trigger helpful repair processes; the story isn’t black and white.
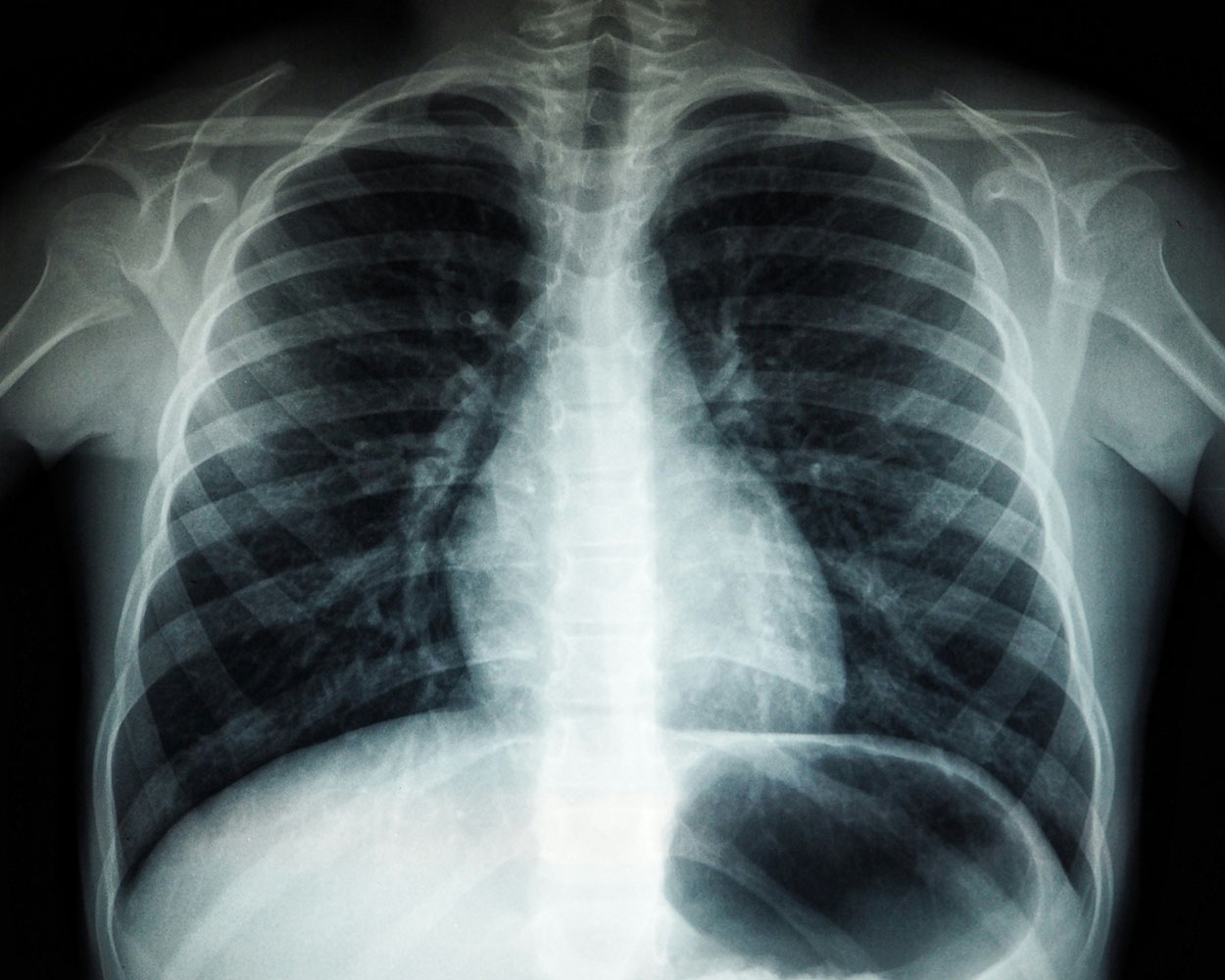
X-rays and CT Scans
X-rays are the backbone of medical imaging. From plain radiographs to mammograms and CT scans, they let doctors see bones, lungs, and much more without surgery. Together, X-ray-based tests constitute the bulk of imaging performed in hospitals. Newer CT scanners deliver faster, sharper results, helping clinicians diagnose injuries, cancers, and organ problems more accurately.
PET Scans and How the Body Works
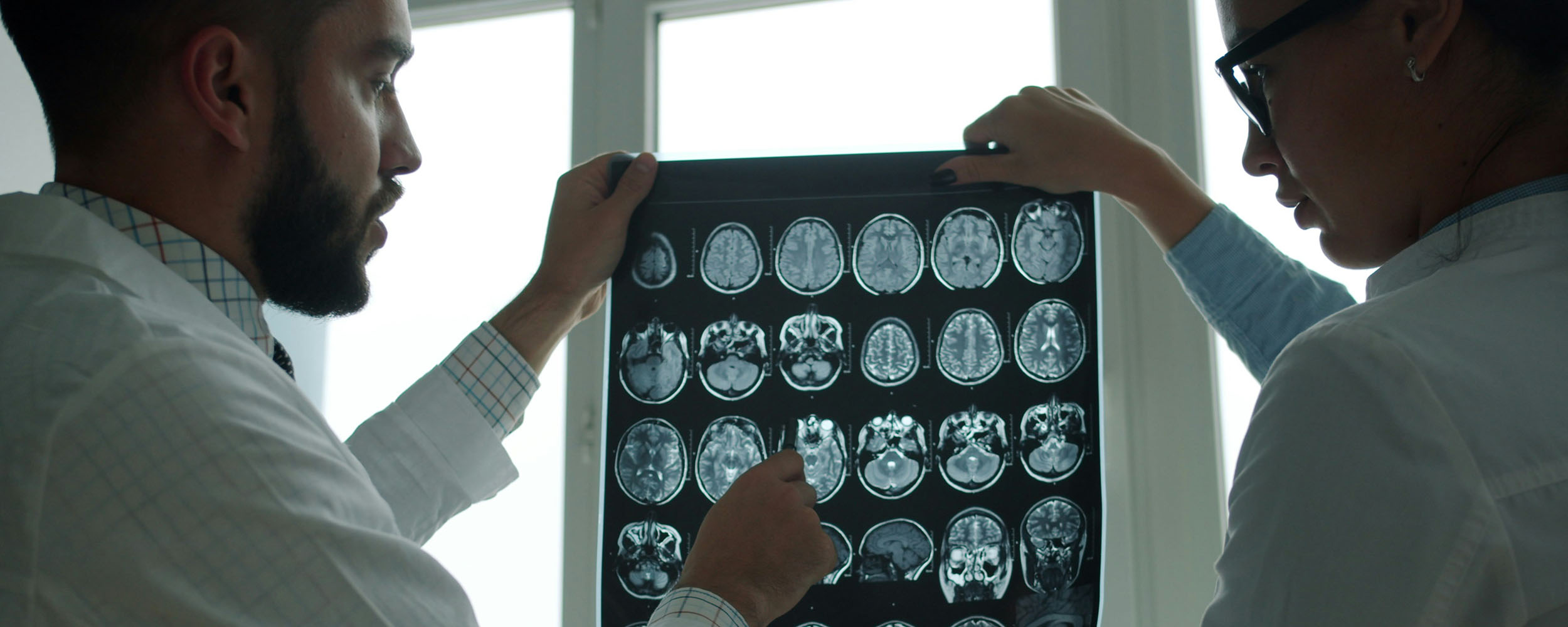
If X-rays show what something looks like, PET scans (Positron Emission Tomography) show how it behaves. Before the scan, patients receive a small harmless radioactive tracer, and the scan reveals how tissues use energy. That’s hugely helpful in oncology, where PET scans can be used to spot active tumours or show whether a treatment is working. Interestingly, when PET is paired with CT, doctors get both functional and structural information in a single image.
MRI Scans and Emerging Non-Ionising Tools
Magnetic Resonance Imaging (MRI) uses magnets and radio waves instead of ionising beams, so it’s safer for repeated use. It is the imaging modality of choice for seeing soft tissues such as the brain, muscles, and joints with great clarity. The downside of MRIs is that they can be expensive, time-consuming, and noisy, and they’re not suitable for everyone, especially people with certain implants or claustrophobia.
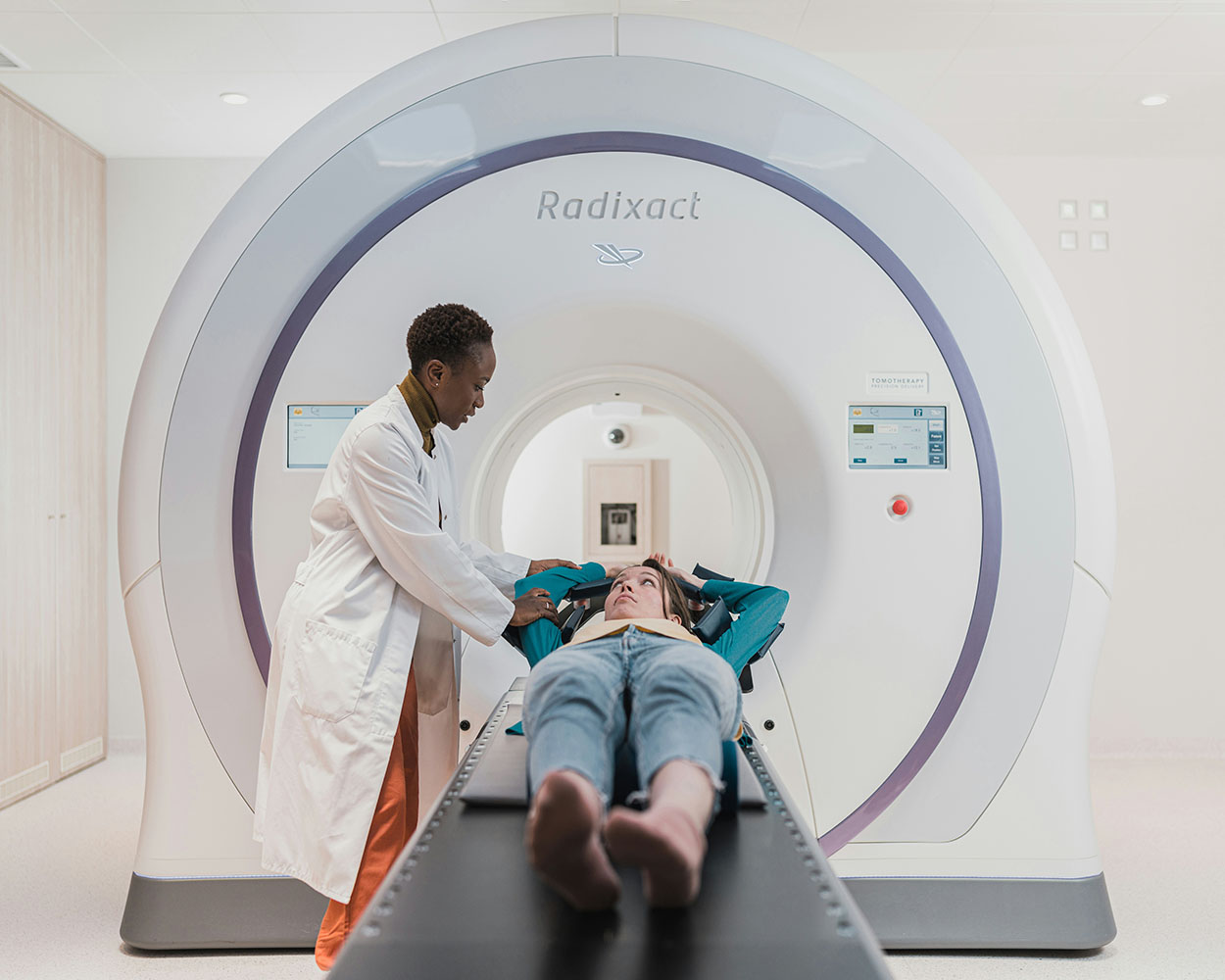
Still, MRIs show that not all imaging relies on ionising energy. Researchers are exploring techniques like microwave imaging to detect early tumours or strokes, while infrared therapies may help alleviate pain. These approaches show that lower-energy waves can still be medically useful, although researchers must always adhere to the safe exposure limits.
Radiation as Treatment
Radiation isn’t just for seeing what’s wrong – it can also fix it. In cancer care, focused beams of radiation target tumours, destroying cancer cells while sparing surrounding tissue as much as possible.
Around half of all people with cancer will receive radiation therapy at some point. Scientists are now developing medicines and genetic techniques to make cancer cells more sensitive to radiation, improving results and reducing side effects.
The Bottom Line: Use with Care
Radiation has become woven into modern medicine because it works. The ongoing challenge is straightforward: get the benefit, limit the risk. With smart guidelines, better technology, and wise use, radiation can continue to help diagnose and treat diseases while keeping patients safe from its detrimental side effects.
Andre Mifsud is a third-year student in the Faculty of Medicine and Surgery. For his second-year physiology research project, conducted under the supervision of Chev. Prof. Renald Blundell from UM’s Department of Physiology and Biochemistry, he investigated the role of radiation in human health.




Comments are closed for this article!